Locations and Care
![]()
Whether you’re home or away, find a location closest to you. Search by facility.
Logan Services
Logan Health offers a wide variety of services and care. Please select from the dropdown below to see more specific to your health care needs.

Our people are everything. The amazing providers, employees, and volunteers at Logan Health gift this organization with their innovation, knowledge, and compassion. Together, we’re connecting our community to trusted, quality care and helping to improve lives every day.

By offering high-quality health care, responding to community needs, and concentrating resources in areas that truly make a difference, Logan Health maintains a rich tradition of giving back to the communities we serve.
Logan News & Events
![]()

46th Annual A.L.E.R.T. Banquet Patient Story: Trooper Lewis Johnson
Montana Highway Patrol Trooper Lewis Johnson was critically injured during a police chase near Eureka in February 2023. In a remote area with life-threatening injuries, time was of the essence to get him to a hospital. Thanks to the coordinated efforts of Eureka EMS, the Lincoln County Sheriff’s Office, Montana Highway Patrol, and other local agencies, Trooper Johnson was swiftly taken to a Ranger Station, where A.L.E.R.T. was ready to assist. This story highlights the vital role of the A.L.E.R.T. program, both in rescue operations and transport logistics.
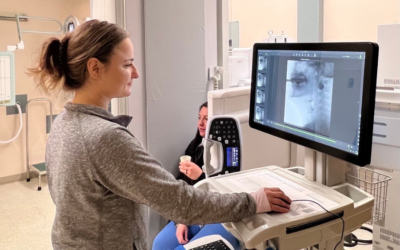
New radiology equipment impacts the field of speech language pathology
Logan Health – Shelby’s recent installation of new Shimadzu Digital Radiology equipment includes the only innovated Fluoroscopy unit available in the region. Fluoroscopy is a type of medical imaging procedure that shows a continuous X-ray image on a monitor, much like an X-ray movie. With this new technology, Modified Barium Swallow Studies (MBSS) are available at Logan Health – Shelby.
Logan Health awards Healthy Classrooms grants to 19 Flathead Valley educators
Logan Health’s Foundation and School-Based Services awarded $500 grants to 19 educators at Flathead Valley schools this April. The Healthy Classrooms Grant provides funding to local schools to aid in the creation or improvement of student-centered and staff-related healthy living initiatives.
Community Impact: Health and Safety Education
By offering high-quality health care, responding to community needs, and concentrating resources in areas that truly make a difference, Logan Health maintains a rich tradition of giving back to the communities we serve.